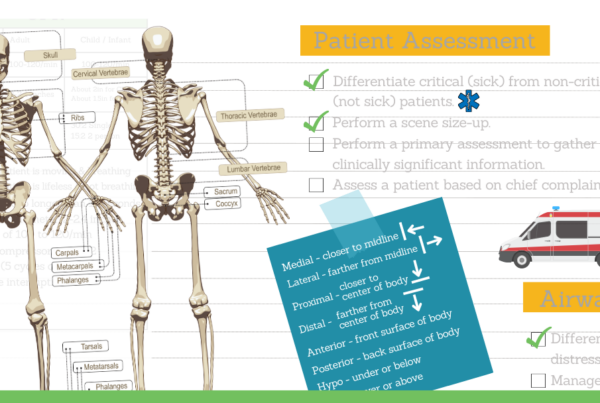
By Dan Limmer
One of the ways I keep up with emergency medicine is by subscribing to emails from emergency medicine publishers and websites, with Medscape and Lippincott being two good examples. They provide an overview of recently published research papers, many of which are relevant to EMS. I always scan the emails for topics of interest in my practice and frequently look at the original paper the article is based on.
Seizure and Syncope Differential Diagnosis
One example I recently saw is the following article: Clinically Differentiating Seizure from Syncope
This caught my eye because I am fascinated by the concepts of differential diagnosis and assessment. The paper told me things I knew, like lip smacking, auras and tongue biting seemed to indicate seizure. A prolonged period of altered mental status also tended to indicate seizure. One thing surprised me. I had always believed that incontinence was a pretty reliable indication of seizure in a patient who had experienced altered mental status when bystander and family reports were inconclusive. It turns out that — in this small group of patients — incontinence was more likely to occur in syncope than seizure.
As I digested this information I thought about how it might change my thinking and diagnosis. I also wondered how this might be digested by others in EMS. EMS providers often struggle with things perceived as ambiguous or without detailed clinical application.
If I were to summarize my impressions of the article, I would say:
- even hospital clinicians have difficulty differentiating seizure from syncope,
- patients present wildly differently even with the same underlying condition and
- there seem to be few smoking guns as clues in these cases.
Each patient has to be evaluated and treated according to their individual presentation. I now know additional things to look for and a better sense of the clinical validity of each sign or symptom alone.
Given this information, would everyone come to the same conclusions? Probably not—and that’s OK. Yet in EMS we often have trouble with gray areas or inconclusive statements. There are three broad stroke ways that this material may be misinterpreted or written off:
- It doesn’t apply to EMS – this is a paper based on hospital practice and neurological specialists.
- It isn’t conclusive – if it doesn’t tell me how to tell a seizure from syncope, it doesn’t help me.
- Making false assumptions – So next time I see incontinence, it is syncope. Right?
Not all research papers (or textbooks for that matter) provide everything you need to know about a topic. It is up to the reader to carefully read, analyze, think and apply each bit of information to clinical practice. It combines with experience and existing knowledge to form that mature approach to practice.
Using Medical Research in the EMS Classroom
If you are an educator reading this blog post, put the linked article up on the screen in your next class and ask your students to write down (anonymously) what they learned from the article and how they believe it applies to their practice of EMS. Collect the answers, read them to get a feel of where your students stand, then discuss the article in class.
We’d love to hear how it goes!
For more ideas on using medical research, scholarly articles and FOAMed in EMS classrooms, visit 6 Way to Use FOAMed in Your Classroom.